FELINE CARDIOMYOPATHY
What is cardiomyopathy?
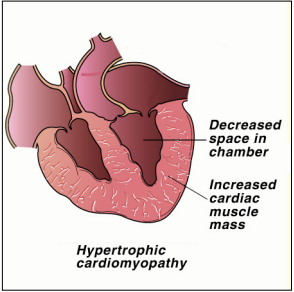
Cardiomyopathy is the name for several diseases of the heart muscle – cardio refers to the heart, myo means muscle. In cats, three classes of cardiomyopathy have been described: hypertrophic, dilated and intermediate (restrictive). In all three types, the muscle walls that make up the heart are abnormal (either too thick or too thin) and the heart becomes unable to
function normally, resulting in symptoms of heart failure. Cardiomyopathy may be seen as a primary condition that is genetic or inherited, or secondary to other diseases that damage the heart. This disease affects 1 in 6 cats to some degree.]
Dilated cardiomyopathy, or DCM, where the heart muscle wall becomes thin and stretched, is now rare since the discovery of taurine as an essential nutrient for cats. Taurine is an amino acid
important to heart development and function. Before the early 1980’s, no one knew that taurine needed to be supplied in cat food and millions of cats developed heart failure because of
insufficient taurine. Now DCM is mostly seen in cats who are eating a homemade or poorly formulated diet, or in rare cases where it is genetic.
Most of the forms of cardiomyopathy we see today is the hypertrophic forms, HCM. There aretwo main types:
• Genetic, inherited HCM starts when a cat is young and is often severe and fatal.
• Acquired HCM, seen in older cats, may be secondary to valve disease or hyperthyroidism, and is usually milder.
What are the signs seen with cardiomyopathy?
In the early stages of disease, the cat may not show any signs of disease. This is referred to as compensated heart disease. The heart is not normal but there are no obvious signs of disease. Cats are good at masking their symptoms and owners often do not notice that the cat is tiring quickly or has a rapid heart rate.
Often cats will alter their activity levels to cope with their disease, which makes it difficult to diagnose cardiomyopathy until it is quite advanced.
Cats with cardiomyopathy are high risk for anesthesia. Sudden death while having an anesthetic procedure is not uncommon, and in fact cardiomyopathy is the number one reason for anesthetic deaths in cats.
Many cats with cardiomyopathy have heart murmurs that would indicate there is a problem.
Hearing a heart murmur will usually prompt us to recommend further heart testing but these
murmurs are often soft and difficult to hear, and 1/3rd of affected cats don’t have a murmur at all. Cats who have hyperthyroidism or high blood pressure from kidney disease are also at higher risk for heart disease and can develop heart murmurs as well, with or without cardiomyopathy.
The major long term concerns with all types of cardiomyopathy are:
1. Development of congestive heart failure: Breathlessness and lethargy are the most frequently noticed signs of congestive heart failure. They result from failure of the heart to efficiently pump blood. The cat tires easily and has little energy for play. He or she may pant or breathe with the mouth open, especially when stressed. Breathing may appear labored.
Not all cats will show signs that owners can see, even when the heart function is poor.
HEART DISEASE =
The heart has structural abnormalities, but it still maintains its ability to pump blood adequately.
HEART FAILURE =
The diseased heart can no longer compensate and symptoms are
appearing, such as trouble breathing and exercise intolerance.
Many cats are found dead by their owners without any prior signs of disease.
2. Thromboembolic disease: When the blood is not flowing properly through the heart blood clots can form within the heart, which is called a thrombus. If parts of the thrombus
become dislodged, they can travel in the bloodstream and block smaller blood vessels. These travelling blood clots are called emboli.
The most common place for emboli to lodge is at the bottom of the aorta, which is the largest artery in the body. This results in obstruction of the blood supply to the back legs,
which is very painful and leads to paralysis. Although some cats may recover with appropriate treatment, this is a potentially fatal complication of any type of
cardiomyopathy.
3. Hypertension: High blood pressure, or hypertension, is a possible complication seen in many cases of hypertrophic cardiomyopathy. This may result in spontaneous bleeding,
such as nose-bleeds or hemorrhage within the eye, and may cause retinal detachment and blindness. This may be noticed as a sudden loss of vision and widely dilated pupils. This is an emergency situation since the blindness will be permanent unless the retina is reattached within a couple of days. Strokes affecting various parts of the brain are also seen from hypertension.
Drugs that lower the blood pressure may be used to treat cats with this problem. Measuring blood pressure in cats can be difficult due to the rise in blood pressure that
occurs with stress, which makes interpretation of results difficult. Most cats are stressed when they are here. Examination of the eyes may give early indications of hypertension since the blood vessels of the retina may show changes and small hemorrhages may be
seen.
How is cardiomyopathy diagnosed?
Heart disease can be suspected if the cat has signs of heart disease, or it may be found on chest x-rays, electrocardiography (ECG) or a cardiac ultrasound scan (echocardiogram). Not all
forms of cardiomyopathy can be diagnosed on an ECG or chest x-ray. Echocardiograms are expensive and not readily available as a pre-screening tool for anesthesia.
Cardiopet® proBNP is a relatively new screening blood test for HCM. The ProBNP enzyme is released from heart muscle cells in response to wall stress. When the cells are stretched or
damaged they start leaking muscle enzymes. The more stressed or damaged the muscle the higher the levels will be. Test results will be normal, mildly high or high.
ProBNP can be a frustrating test to interpret. In the cat, there is a fairly large overlap between normal and abnormal levels, so when we get a ProBNP level around the high end of normal we can’t be sure if the cat is normal or has early disease. If the cat has
HCM and we wait a year to check it again our patient may already be in heart failure. If a cat seems normal but the proBNP level is in the mildly high range, we will wait 3 months and test it again. If
heart disease exists, the enzyme level should continue to go up and we will know it’s time for an echocardiogram.
An echocardiogram is an ultrasound of the heart. The sound waves bouncing off the heart tissue let us see the heart beating and measure the thickness of the muscle walls. We can also measure the contractility of the heart – how effectively the heart is squeezing blood into the arteries. An echocardiogram is the only way to definitively
diagnose cardiomyopathy and completely assess heart function. Unfortunately, it’s too expensive to use as a routine screening tool.
Here at Best Friends, we have an internal medicine specialist who comes to do echocardiograms (commonly called echoes), or we can refer you to a cardiologist at Lakeshore
Veterinary Specialists. In cases where hypertension is a possibility, the blood pressure will be evaluated. Retinal examination may provide evidence of hypertension where blood pressure measurements cannot be made. Specific tests may be done in order to check that the cardiomyopathy is not secondary to some other disease, such as thyroid and kidney disorders.
What causes cardiomyopathy?
Cat breeds with higher risk for cardiomyopathy include:
Abyssinian
American short hair
British short hair
Cornish and Devon Rex
Domestic short hair
Domestic long hair
Maine Coon
Persian
Ragdoll
Siamese
There are many causes of cardiomyopathy. In older cats, as
already mentioned, thyroid disease (hyperthyroidism) commonly causes cardiomyopathy. Genetic forms of cardiomyopathy occur in some breeds of cats, especially Ragdolls and Persians. These cats often have a very short life expectancy and can die as young as a few months of age.
An echocardiogram may be recommended at 6 months of age and then every 6 months thereafter to screen for the disease in susceptible breeds. We now have DNA tests breeders and pet owners can use to screen for some of these genetic forms of HCM.
How is cardiomyopathy treated?
In cases where an underlying cause of the heart disease is found, treatment of that problem
may result in improvement or reversal of the heart disease. Hyperthyroidism is the most treatable
cause of cardiomyopathy, since complete resolution of the heart disease is possible if it is
diagnosed and treated early. In cases where no cause is identified (referred to as idiopathic
cardiomyopathy), and in cases where the disease persists following treatment for an underlying
cause, then medication may be needed.
Treatment varies according to each case but may include many medications also used in
humans:
- Diuretics if congestive heart failure is present.
- Beta blockers to reduce the heart rate where this is excessive.
- Calcium channel blockers to help the heart muscle relax and hence help more effective
filling of the heart. - Aspirin or a drug called clopidogrel may be used to reduce the risk of thrombus formation and thromboembolic disease. Dosing of aspirin should always be as advised by a veterinarian since aspirin may be toxic to cats. Aspirin poisoning, which occurs if the dose or frequency of aspirin administration is too high, may cause vomiting and internal
bleeding. If your cat shows these signs, stops eating or appears sick, aspirin therapy should be stopped and you should consult your veterinarian immediately. - ACE inhibitors – these drugs also help to control congestive heart failure.
- Primobendan, a drug that helps the heart to contract more effectively.
The long term outlook for a cat with cardiomyopathy is extremely variable depending on the cause of this disease. Cats with idiopathic cardiomyopathy may remain stable for several years.
Those with the inherited forms are usually the most severely affected.
Does a cat with cardiomyopathy need a special diet?
Low sodium therapeutic diets are recommended for cats with cardiomyopathy. This may decrease the risk of developing congestive heart failure and hypertension. We have several brands to choose from. Cat treats and over-the-counter diets are often quite salty and should
be avoided.
